Cassie Warren is a health educator, activist and youth worker dedicated to radical access to affirming health services, especially for trans and queer young people. She works at the Broadway Youth Center in Chicago–a community space for trans and queer youth experiencing homelessness.
Last month, Cassie was invited by UNICEF to speak on a panel about PrEP, a new pill that prevents the acquiring of HIV. They took the opportunity to address publicly not merely the barriers that keep trans and queer young people–particularly those of color–from getting on PrEP, but the structures of US healthcare that purposefully deny effective and affirming care for oppressed people at large. Here is what they had to say:
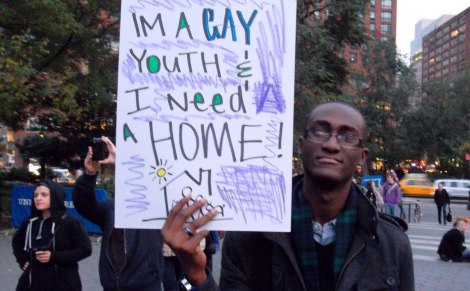
Queer youth reminding us what the real barriers to healthcare are.
Today, I will be speaking from my current experience and relationships with young people. I help young folks navigate the American healthcare system, and provide supportive services and resources to primarily Black, trans and queer young people experiencing homelessness in Chicago, at a community space called the Broadway Youth Center.
I hope that I can contribute to this convening by illuminating the policy changes that could remove some of the barriers in writing PrEP prescriptions for young people, and the demands we should be making of our healthcare system when it comes to creating a landscape where PrEP is accessible to all young folks.
The successes I share with you today are largely due to the frameworks we use and our model of care.
We provide integrated social and medical services in a center that only serves young people. We believe there should be multiple points of access to these services. A young person may come to our space to get a hot meal, a state ID voucher, or to get some sleep, and they may stay or come back for community meeting, an HIV test, or our GED program. We believe young people are the experts in their own lives and position ourselves as resources or as advocates for the resources they tell us they need.
We think there should be as few barriers as possible to accessing health care, that your documentation status doesn’t matter, that young people know what’s best for themselves, and that all gender expressions are valid, important, deserving of celebration. We utilize harm reduction, strengths-based, and transformative justice approaches to all our work.
Because of the context and setting in which we provide our services, we are able to make them accessible to the folks most likely to be turned away or banned from other social and health services. Yet, we still experience structural barriers that keep us from getting PrEP to the folks interested in starting. Three concrete policies whose support could remove some of these barriers and benefit young people are:
- People under 18 need to be actively included in trails that are fortifying PrEP access nationally and internationally.
- The creation of medication assistance programs for young people who are on their parent’s health insurance, but don’t want to use it because of the physical, emotional, or economic risks tied to depending on their biological families.
- Same day initiation of PrEP, or getting folks who express interest on the pill as soon as possible.
However, while these policy changes would put us in a place to provide a prescription for young people, successful PrEP access and use is not just about writing a prescription. It is about creating real paths to affirming healthcare for the young people most at risk of acquiring new HIV infections: Young, Black, trans and queer people, a significant number of whom are homeless.
I’d like to talk about the things that are integral to address when we are working together to support youth in accessing and taking PrEP successfully.
The young people I’m speaking of face significant barriers to basic resources on a daily basis, even outside of the barriers inherent within the US healthcare system. A lack of stable housing means a lack of storage, lack of security for your belongings, and a constant preoccupation with and hyper awareness of your surroundings. It means stress and anxiety stemming from not knowing where your next meal might come from, to constant surveillance and harassment by police. It often means you don’t have regular access to personal documentation, like an ID, social security card or birth certificate.
When I hear folks in healthcare concerned about young people adhering to the regiment of a medication like PrEP, I don’t often hear them talking about the structural oppressions that make adherence difficult to impossible: Lack of safe storage; the bureaucracy around Medicaid that makes it so easy to lose care; being denied services based on gender markers, or a new name that doesn’t match medical records; not having state ID, a social security number, or other documentation; lack of bus fare to pick up or refill prescriptions; the criminalization of survival crimes and/or quality of life crimes; limited access to a consistent phone number or email; the lack of youth-only spaces.
Within the US healthcare system there are mountainous barriers for Black, Brown, trans and queer young people–costs, required ID, not to mention care often is not gender-affirming, and rarely gives youth the ability to consent to their own healthcare. There is inherent harm and trauma in the medical system, especially for the young people at highest risk for acquiring HIV.
In the US, people without access to health insurance have learned to receive their care at hospitals and ERs. A study conducted by the Young Women’s Empowerment Project in Chicago found that young, Black, trans and queer people report hospitals as the second most harmful institutions in which they experience violence, second only to the criminal justice system.
And really, there is no difference.
When many of these young people attempt to access services at hospitals, they are regularly arrested or institutionalized. I’m going to say that again, because I want to make sure this point is clear:
The populations at highest risk for HIV are poor, young, Black, trans and queer folks, and often, when they attempt to seek services from public outlets, they are arrested or institutionalized.
The US healthcare system is one that often takes away our ability to have options and control over our own health, a place where many people feel shamed for their lifestyle choices, and where power dynamics are rarely in the favor of young people, people of color, trans and queer people. But PrEP should challenge all of these things.
PrEP and shame do not go together. PrEP is a new option we can offer young people. PrEP gives power and control to the receptive partner.
Often, because of the heirarchical structures valued by our healthcare system, the inherent abilities of young people are erased. But if we take the time to see their strengths, to recognize and defy those structural barriers, we are able to figure out how to meet folks where they are, and return some of their power to them. We cannot talk about successful uptake of PrEP and young people without being strengths-based, without being sex-positive, without being youth-centered, and without giving youth the ability to identify and address all their health needs.
The challenges surrounding offering PrEP to young people should not be seen as threats, but instead as opportunities. For they shine light on the inadequacies of our healthcare system, and bring into sharp focus the barriers we need to address and remove.
We have a highly effective, safe pill we can take to prevent HIV. But PrEP only works when we are given real access to it.
If trans folks are the most vulnerable population, and we don’t have trans competent doctors, we create barriers to access. If we arrest or institutionalize poor, Black young people for attempting to seek the care they need, we create barriers to access. And without access to take it, PrEP cannot work.
If we want young people to take PrEP, to get engaged in primary care, then we have to provide gender affirming services. We have to get rid of security guards and police in our healthcare clinics. We need to affirm young people’s consensual pleasures. We need more youth-only healthcare spaces, and insurance companies need to survive on something other than capitalism.
Last week at the exact same time that marriage equality passed in the United States, a vibrant, courageous, young trans person I work with was killed. This is crucial to note, because the successful advancement of policy does not equal the distribution of resources that are affirming, safe and accessible to all, especially those at the intersections of multiple oppressed and policed identities.
Ending HIV is bigger than policy, bigger than the healthcare system alone. It is about ending prisons and detention centers as the primary places people receive housing and healthcare. It is about centering trans leadership across movements and communities. It is about a commitment to strong social services, including public education, child care, and reproductive freedom. It is about the decriminalization of street economies, of sex work, of homelessness. It is about ending all forms of violence that treat Black, trans and queer communities as undeserving of love, of respect, of care.
There is a clear, continued pattern, a pattern in which healthcare policy and practices uplift folks who are already privileged to have access to more resources that lower their risk, and provide them more support. At the last several PrEP summits I’ve attended, researchers talk about the outstanding number of people lining up for PrEP, but say that they are rarely the folks most at risk for acquiring HIV.
The time to recognize the barriers and challenges facing young, Black, trans and queer youth and respond in ways that are supportive, humanizing, and focused on their voices, is now.
PrEP can help all of us get to zero, or it can merely help certain communities with access get to zero. It can ramp up care for the communities that have always been most impacted by the HIV virus, or it can further widen the gap in racial, economic, and gender disparities that continue to fuel the HIV epidemic.
Now is the time to decide to be on the right side or wrong side of justice. PrEP works, but only when we actively dismantle the barriers to young folks’ access to it.

Reblogged this on Fairy JerBear's Queer World News, Views & More From The City Different – Santa Fe, NM and commented:
An important look at the myriad difficulties faced by those at risk of HIV infection who could benefit from PrEP and the need to address the barriers and challenges faced by young trans and queer youth of color.
Reblogged this on Project Safe.
Pingback: 16 HIV Advocates to Watch in 2016 | HIVPlusMag | PozitiveHope·